 July 1, 2023
July 1, 2023
Did you know that our skin is the largest organ in our body? Yet more often than not we tend to ignore it or not pay much attention to it. Ringworm is a common fungal infection that has plagued our society for a long time now. But not enough people are aware of its effect on our bodies and how they can prevent themselves from contracting it. It’s time we educate ourselves more about this highly preventative disease.
Ringworm, also known as dermatophytosis, is a common fungal infection that affects the skin, nails, and hair. Despite its name, ringworm is not caused by worms but by a group of fungi called dermatophytes. These fungi feed on the keratin protein found in the outer layers of the skin, hair, and nails, leading to the characteristic symptoms of the infection.
The term "ringworm" is derived from the appearance of the infection on the skin. It often presents as a red, circular rash with raised edges and a clear centre, resembling a ring. However, the appearance may vary depending on the location of the infection and the individual's immune response.
Ringworm is highly contagious and can be transmitted through direct contact with an infected person, animal, or object. Common sources of infection include contact with infected animals such as cats and dogs, sharing personal items like towels or combs, and contact with contaminated surfaces in public places like locker rooms or swimming pools.
To diagnose ringworm, a healthcare professional may perform a visual examination of the affected area and may also take a sample for laboratory testing. Microscopic examination and culture of the sample can help identify the specific fungus causing the infection.
Ringworm, also known as dermatophytosis, is a specific type of fungal infection caused by dermatophytes, which are a group of fungi that infect the skin, hair, and nails. While ringworm shares similarities with other fungal infections, there are distinct differences that set it apart.
Ringworm is primarily caused by dermatophytes, specifically three main species: Trichophyton, Microsporum, and Epidermophyton. These fungi have the ability to invade the keratinized tissues of the body, including the skin, hair, and nails. In contrast, other fungal infections, such as candidiasis or yeast infections, are caused by different types of fungi, predominantly Candida species. Candida infections typically affect the mucous membranes, such as the mouth, genital area, or moist skin folds.
Ringworm infections present distinct clinical features. The characteristic symptom of ringworm is the presence of a circular rash with a raised, red border and a clear centre, which resembles a ring. This appearance is the reason behind the name "ringworm." The affected area may be itchy, scaly, and may sometimes have blisters or pustules. On the other hand, other fungal infections may manifest as red, scaly patches, plaques, or nodules, but they do not typically exhibit the classic ring-like appearance seen in ringworm.
Ringworm is highly contagious and spreads through direct contact with infected individuals, animals, or contaminated objects. It can also spread indirectly through contact with surfaces in public places like locker rooms or swimming pools. Sharing personal items, such as towels, clothing, or combs, can facilitate transmission. In contrast, other fungal infections are generally not as contagious and often result from overgrowth of fungi already present on or within the body, or from exposure to fungal spores in the environment.
Ringworm can affect various parts of the body, including the skin, nails, and scalp. In contrast, other fungal infections, such as candidiasis, tend to occur in specific areas, such as the mouth (oral thrush) or genital region (vaginal yeast infections in women or balanitis in men).
The treatment of ringworm involves the use of antifungal medications, which can be administered topically or orally, depending on the severity and location of the infection. Topical antifungal creams, ointments, or powders are commonly used for mild cases, while oral antifungal medications may be prescribed for more severe or widespread infections. Treatment duration typically ranges from a few weeks to several months, depending on the site and extent of the infection. In contrast, other fungal infections may require different antifungal medications or alternative treatment approaches, depending on the specific fungus involved and the affected area of the body.
Ringworm, being a contagious fungal infection, can affect individuals of all ages and backgrounds. However, certain factors can increase the susceptibility of certain individuals to developing ringworm. Here are the groups of people who are more prone to ringworm infection:
Children, particularly those in close contact with infected individuals or animals, are more susceptible to ringworm. This is because their immune systems are still developing, and their frequent participation in activities that involve close physical contact or sharing of personal items (such as toys, clothing, or sports equipment) increases the risk of transmission.
Athletes and individuals who engage in sports or physical activities that involve close skin-to-skin contact, prolonged sweating, or the use of communal facilities (such as locker rooms or showers) are at higher risk of developing ringworm. These activities create an environment that promotes the transmission of the fungal infection, particularly in areas prone to moisture, such as the feet (athlete's foot or tinea pedis) or groin (jock itch or tinea cruris).
People with weakened immune systems, such as those with HIV/AIDS, undergoing chemotherapy, or taking immunosuppressive medications, are more susceptible to various infections, including ringworm. A compromised immune system reduces the body's ability to fight off fungal infections effectively, making these individuals more prone to developing ringworm.
Ringworm is highly contagious and can spread through direct contact with infected individuals or animals. People who live or work in close proximity to individuals or animals with ringworm have an increased risk of contracting the infection. This includes family members, roommates, healthcare workers, and individuals working in animal shelters or veterinary clinics.
Certain occupations or environments may increase the risk of developing ringworm. For example, individuals working in professions that involve frequent contact with soil, such as gardeners or farmers, may have an increased risk of contracting ringworm from the soil or animals they handle. Similarly, individuals working in humid environments, such as swimming instructors or lifeguards, may be more prone to developing fungal infections like athlete's foot.
While these groups of people are more susceptible to ringworm, it is important to note that anyone can develop a ringworm infection.
Symptoms of ringworm can vary depending on the location of the infection on the body. Here are the common symptoms to look out for when suspecting a ringworm infection:
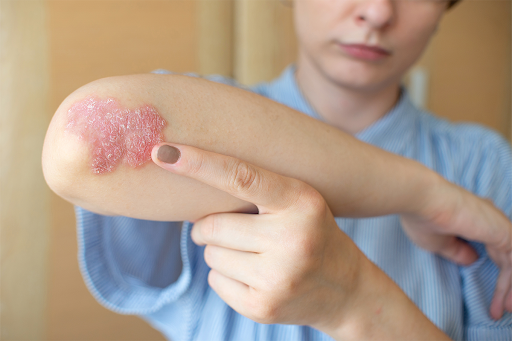
Tinea corporis, also known as ringworm of the body, typically presents as a red, scaly rash that gradually expands outward. The affected area often forms a ring-shaped pattern with raised, well-defined edges and a clearer centre. The rash may be accompanied by itching, and it can appear on various parts of the body, including the arms, legs, trunk, and face. In some cases, small blisters or pustules may develop within the affected area.
Tinea capitis refers to ringworm of the scalp, which primarily affects children. Common symptoms include patches of hair loss, scaling, and itching. The affected areas may appear red or black, and the hair near the infection site can become brittle or break easily. In some cases, there may be swollen lymph nodes in the neck, and the scalp may have pus-filled sores.
Tinea pedis, commonly known as athlete's foot, primarily affects the feet. Symptoms can include itching, burning, and stinging sensations, especially between the toes. The skin may become red, scaly, and flaky, with blisters or ulcers forming in severe cases. Athlete's foot can spread to the soles of the feet, causing dry, thickened skin with deep cracks or fissures.
Tinea cruris, also known as jock itch, affects the groin area. It commonly occurs in males but can also affect females. Symptoms include a reddish-brown rash with well-defined edges and raised borders. The affected area may be itchy, with a burning or stinging sensation. The rash can extend to the inner thighs, buttocks, and genitals. In some cases, there may be flaking or peeling of the skin.
Tinea unguium, also known as onychomycosis, affects the nails, particularly those on the hands and feet. Symptoms include thickened, discoloured (yellow or white), and brittle nails. The nails may become distorted in shape and can develop a crumbling texture. In severe cases, the nails may separate from the nail bed, causing pain or discomfort.
It is important to note that these symptoms may not be exclusive to ringworm and can be seen in other skin conditions as well. If you suspect a ringworm infection based on the symptoms mentioned above, it is recommended to consult a healthcare professional for an accurate diagnosis and appropriate treatment.
The treatment of ringworm depends on the severity and location of the infection. It generally involves the use of antifungal medications, which can be administered topically or orally. Here are the common treatment approaches for ringworm:
For mild to moderate cases of ringworm, topical antifungal creams, ointments, or powders are often recommended. These medications are applied directly to the affected area and surrounding skin according to the instructions provided by the healthcare professional. Commonly used topical antifungals include:
a. Clotrimazole: Available over-the-counter, clotrimazole is an effective antifungal agent used to treat various types of ringworm infections.
b. Terbinafine: Terbinafine is available as both prescription and over-the-counter formulations and is effective against most types of dermatophytes.
c. Miconazole: Miconazole is available in various formulations, including creams, powders, and sprays, and is commonly used for ringworm treatment.
It is important to follow the recommended treatment duration and instructions for the proper application of the topical medication.
For more severe or widespread cases of ringworm, oral antifungal medications may be prescribed. These medications are taken by mouth and work systemically to treat the infection from within. Oral antifungals are often recommended for scalp infections (tinea capitis) or cases where topical treatments have not been effective. Commonly prescribed oral antifungals include:
a. Griseofulvin:
Griseofulvin is an oral antifungal that has been used for many years to treat ringworm. It is particularly effective for scalp infections.
b. Terbinafine:
Terbinafine is available in oral form and can be used for various types of ringworm infections.
c. Itraconazole:
Itraconazole is another oral antifungal medication that may be prescribed for severe or resistant cases of ringworm.
It is important to take oral antifungal medications as prescribed by the healthcare professional and complete the full course of treatment to ensure the complete eradication of the fungus.
In addition to antifungal medications, certain adjunctive measures can help manage and prevent the spread of ringworm:
a. Keep the affected area clean and dry:
Gently wash the infected area with mild soap and water, and ensure it is thoroughly dried afterwards. Avoid sharing towels or other personal items.
b. Practice good hygiene:
Wash your hands thoroughly after touching the affected area or applying antifungal medication. This helps prevent the spread of the infection to other parts of the body or to other individuals.
c. Avoid scratching:
Although ringworm can be itchy, scratching can worsen the condition and increase the risk of spreading the infection. Try to resist the urge to scratch or pick at the affected area.
d. Launder-contaminated items:
Wash any clothing, towels, or bedding that comes into contact with the infected area in hot water to eliminate any fungal spores.
e. Prevent re-infection:
If you have pets with ringworm, consult a veterinarian for appropriate treatment. Avoid contact with infected animals until they have been treated and declared ringworm-free.
It is important to note that self-diagnosis and self-medication may not always be accurate or effective in treating ringworm. It is recommended to consult a healthcare professional for proper diagnosis and treatment.
Preventing ringworm infection involves adopting good hygiene practices and taking precautions to minimize the risk of exposure to the fungus. Here are some preventive measures to consider:
● Keep your skin clean and dry: Regularly wash your body with soap and water, paying attention to areas prone to sweating, such as the armpits, groin, and feet. Dry your skin thoroughly, especially in skin folds, to prevent moisture buildup.
● Wash your hands: Thoroughly wash your hands with soap and water, especially after touching animals, using communal facilities, or participating in activities that involve close physical contact.
● Limit close physical contact: Avoid direct skin-to-skin contact with individuals who have ringworm or other fungal infections until they have completed treatment and are declared infection-free.
● Take precautions with animals: If you have pets or work with animals, take appropriate measures to prevent the transmission of ringworm. This includes regular grooming, keeping their living areas clean, and seeking veterinary care if any signs of ringworm are observed.
● Keep feet clean and dry: Wash your feet daily with soap and water, and thoroughly dry them, especially between the toes. Use a separate towel for your feet to avoid cross-contamination.
● Wear clean socks and shoes: Change socks and shoes regularly, especially if your feet tend to sweat excessively. Opt for breathable footwear and moisture-wicking socks to keep your feet dry.
● Avoid walking barefoot in public areas: Wear sandals or protective footwear in public places where the risk of fungal exposure is higher, such as locker rooms, showers, and swimming pool areas.
● Do not share personal items: Refrain from sharing personal items such as clothing, towels, hairbrushes, combs, or sports equipment with others, as these items can harbour fungal spores and contribute to the spread of ringworm.
● Launder items properly: If you suspect any of your personal items may be contaminated, wash them in hot water with appropriate detergents to eliminate any fungal spores.
● Keep living areas clean: Regularly clean and disinfect common areas, surfaces, and objects that may come in contact with the skin, such as bathroom floors, countertops, gym equipment, and wrestling mats.
● Avoid sharing bedding: If someone in your household has a ringworm infection, ensure that they have their own bedding and avoid sharing pillows, blankets, or sheets.
Getting the appropriate medical treatment and care is crucial to avoid any associated medical complications.
To book an appointment, contact us at +91-9540 114 114.
2026 © SSB Heart and Multispecialty Hospital.